
Dr. Erin Thorne, ND, IFMCP
Feminine Functional Medicine
Menopause & Hormone Specialist
Virtual in the state of Washington
Naturopathic & HRT Solutions
American Menopause Society Member
Certified Functional Medicine Practitioner in Seattle, Washington
Sound familiar?

Menopause &
Perimenopause
Hot flashes and night sweats disrupting your sleep and energy
Sudden weight gain — especially around your belly
Brain fog, memory issues
Mood swings, anxiety
Vaginal dryness, painful sex, and low libido
Irregular or heavy periods — or periods that never seem to end
Feeling like you’ve lost your “spark,” your motivation, or your identity

PCOS, Irregular Periods, Fertility Struggles:
Missing periods or unpredictable cycles
Unwanted hair growth on the face, chin, chest, or belly
Persistent acne, even in your 30s and 40s
Weight that won’t budge, especially with carb sensitivity
Fatigue that hits like a wall mid-day
Mood changes, depression, or focus
Difficulty getting pregnant or staying pregnant
If any of this sounds like you — you're in the right place.
We utilize functional medicine and specialize in getting to the root cause of hormone chaos so you can finally feel like yourself again.
Watch Intro to Clinic Here
The Feminine Functional Medicine Difference
1. Root-Cause, Woman-Centered Care
Every phase of womanhood deserves personalized, respectful care.— from menstruation to peri/ post-menopause.

2. Comprehensive Functional Lab Testing
Complete Hormone, Thyroid, Cortisol Testing
Gut Health Stool Testing
Nutrient Testing

3. Cutting Edge Therapies
Semaglutide & Metabolic Peptides
Continuous Glucose Monitors (CGMs)
Peptide and HRT Therapy

4. Lifestyle, Mindset Nutrition Plans
Customized for your individual plan and based on your labs, lifestyle, cycle phase, and preferences.
Leave feeling confident in your plan!

5. Step-by-Step Treatment Plans:
Treatment plans utilizing the proprietary functional medicine matrix that evolve with you — we guide, monitor, and adjust as needed.

6. One-on-One Partnership
Compassionate, Respectful Care where you feel seen, heard, and empowered — you are in the drivers seat at all times here.

ABOUT:

Hi, I'm Dr. Erin Thorne
I am a firm believer of walking the walk I talk.
I strive to teach, inspire, and educate my patients on whole body health, and striving for a full life with energy, vitality and joy. I am on a mission to help women thrive
through every transition
...and believe that it's possible.
As a licensed functional medicine doctor and member of the Institute for Functional Medicine, I provide personalized care rooted in science.
My work with midlife women is also guided by standards from the North American Menopause Society, offering holistic, hormone-focused care you can trust.
Services & Specialties:

Menopause & Perimenopause
📊 Comprehensive Hormone Testing
🧠 Mood, Memory & Sleep Support
🔥 Hot Flash & Night Sweat Relief
🏋️♀️ Weight Gain & Metabolism Reset Plans
💉 Advanced Therapies When Needed
📊 Body Composition + Strength Goals
🥦 Targeted Nutrition Protocols
🧬 Bio-Identical Hormone Therapy (BHRT)
💊 Personalized Supplement Regimens
Hormonal Health
🩸 Comprehensive Hormone Lab Testing
📊 Cycle Mapping & Ovulation Tracking
🧬 Fertility Foundations Plan
📅 Period Repair Protocols
🌸 Post-Birth Control Recovery Plans
🥦 Custom Nutrition & Anti-Inflammatory Plans
💊 Targeted Supplement Guidance


Athletic Advantage in
Polycystic Ovaries (PCOS)
📋 Full PCOS Root-Cause Evaluation
🧬 Functional Lab Testing
🧠 Metabolic Strategy for Muscle + Hormone Sync
🍽️ Performance-Driven Nutrition Planning
🏃♀️ Cycle-Syncing for Training & Recovery
💊 Targeted Supplement Protocols
📊 Body Composition + Strength Goals
🩺 Fertility-Respecting Options
CUTTING EDGE THERAPIES
Holistic Weight loss
Semiglutide, Trizepitide, B12)
Peptide Therapies:
Like BPC-157, MOTS-c, CJC/Ipamorelin) to support healing, cellular repair, muscle growth, and fat metabolism.
Glucose Sensor:
Prescriptions and analysis (to identify spikes and crashes impacting hormones.

How it Works:
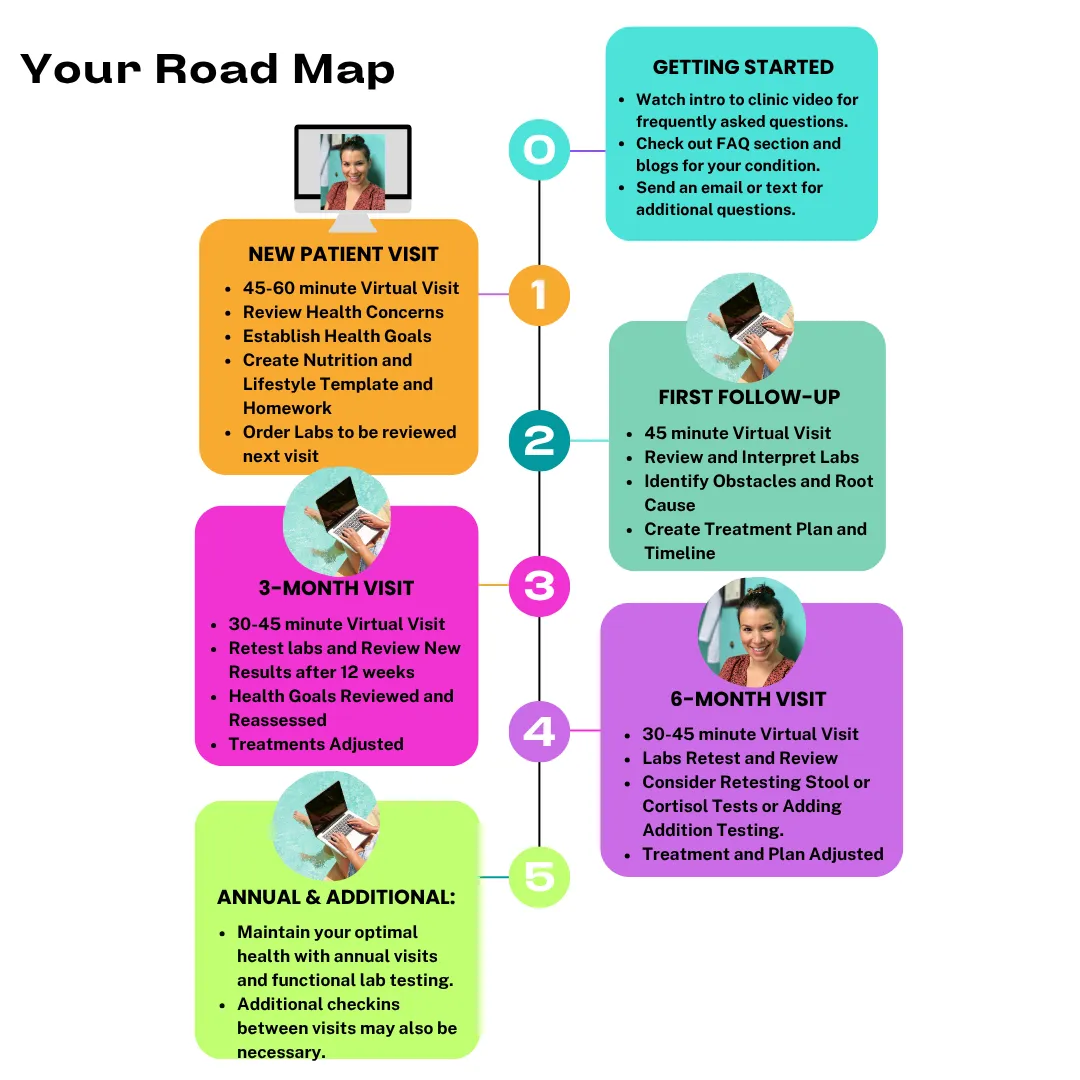
Testimonials:
Frequently Asked Questions (FAQ's):
What are the Costs of Services?
***Dr. Thorne can still order blood work that can be billed to insurance.
However, Dr. Thorne is not in-network with any insurance companies or medicare programs. Dr. Thorne DOES offer a "Superbill" after each visit for patients to submit to insurance for partial reimbursement depending on their healthcare plan.
Payment is still due at time of service.
If you are planning in using a Superbill, you will want to ask your insurance company what the coverage is for an "Out-of-network provider" and what they would cover for a "99204 and/or 99214" coded visit.
Office Visits, Functional Testing & Billing:
New Patient Visit (60 min.) *2 + health concerns: $400
New Patient Visit (45 min.) *1 health concern: $325
A La Cart Pricing:
Follow-up (30 min.): $250
Follow-up (45 min.): $325
Follow-up (60 min.): $400
Quick call: (15. min): $175
Can Dr. Thorne be my Primary Care Physician?
No, Dr. Thorne is not operating as a Primary Care Physician and has instead chosen to specialize in conditions listed above.
Dr. Thorne requires and recommends that all patients see a PCP at least once a year for their annual physical since Dr. Thorne is exclusively virtual.
Does Dr. Thorne Accept Insurance?
***Dr. Thorne can still order blood work that can be billed to insurance.
However, Dr. Thorne is not in-network with any insurance companies or medicare programs. Dr. Thorne DOES offer a "Superbill" after each visit for patients to submit to insurance for partial reimbursement depending on their healthcare plan.
Payment is still due at time of service.
If you are planning in using a superbill, you will want to ask your insurance company what the coverage is for an "Out-of-network provider" and what they would cover for a "99204 and/or 99214" coded visit.
Are there only Virtual Appointments?
VIRTUAL TELEMEDICINE ONLY. Dr. Thorne works with all of her patients virtually. There are no in-person visits available at this time. This is part of the reason that Dr. Thorne recommends or requires that all patients have a PCP do a physical exam at least once a year, and stay on top of mammograms, colonoscopies and other routine exams.
What Type of Hormone Replacement Therapy is Prescribed?
The bulk of HRT prescriptions are available at your local pharmacy and are considered "body identical or bio-identical." This includes: Estradiol patches (topical), sprays and gels for systemic symptoms, and vaginal estradiol cream or tablets for vaginal dryness. Dr. Thorne utilizes oral micronized progesterone shown to prevent endometrial overgrowth while using system estrogen. These therapies are FDA approved and often covered by insurance. For patients requesting compounded medications due to allergies or preferences that option is available as well.
NON-FDA approved therapies for women include topical testosterone cream from a compounding pharmacy and oral or topical DHEA and progesterone.
The medications and hormones listed above are not an inclusive list and there are others not listed.
What is a Functional Medicine and Naturopathic Doctor?
As both a licensed Naturopathic Doctor and a Certified Functional Medicine Practitioner, I bring a unique, integrative approach to hormone health. Naturopathic medicine emphasizes root-cause healing using natural therapies like nutrition, botanicals, lifestyle, and mind-body medicine. Functional medicine builds on this foundation with a systems-based, personalized approach that uses advanced lab testing to identify imbalances and target therapies with precision. For my hormone patients, this means you'll receive deeply individualized care that blends the best of traditional wisdom and modern science—addressing the "why" behind your symptoms, not just the "what," and creating a clear, holistic path to long-term balance and vitality.
Join Dr. Thorne's FemMed Email list!

Let's Get Started!










Facebook
Instagram
X
LinkedIn
Youtube
TikTok